23% of aged care homes will still be in the red despite Budget boost: StewartBrown analysis
The aged care sector’s finances are facing a rocky two years ahead with more homes set to close their doors – even with the Government tipping in an additional $17.7 billion into the system over the next four years – according to...
The aged care sector’s finances are facing a rocky two years ahead with more homes set to close their doors – even with the Government tipping in an additional $17.7 billion into the system over the next four years – according to StewartBrown’s Aged Care Budget Impact Analysis. You can download the report here. The 31-page analysis looks at the impact of the Federal Budget and the Government’s response to the Royal Commission on the aged care sector – and concludes that while the increased expenditure is welcome, it won’t fix the financial viability of the sector.
“While the Budget funding outlays are significant, and some of them will ease the financial hardship of aged care providers, particularly those delivering residential aged care services, the next two years will remain difficult financially,” StewartBrown states.
No funding to cover extra red tape
The accountants also note that many of the new measures are linked to increased reporting, compliance and governance – which isn’t matched with funding for operators to deal with the administrative burden.
“Based on the StewartBrown Survey, administration costs (excluding the cost of the Facility Manager) have risen from an average of $29.16 per bed day in Dec-15 to an average of $37.50 per bed day in Dec-20. These costs are not specifically attached to any single funding stream, however, they have to be paid for and inevitably, as the reporting and compliance obligations increase, the costs will also increase.”
Any wage increase could hit operators hard
There is some good news.
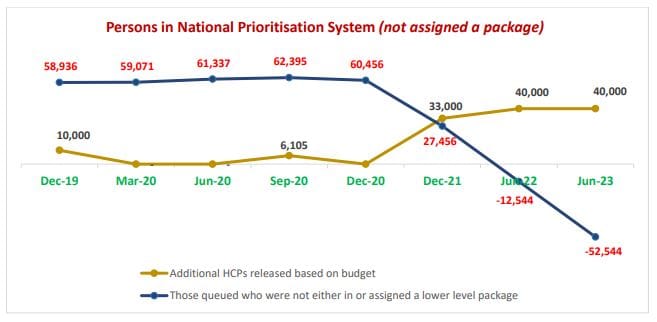
The analysis forecasts that the release of the 80,000 Home Care Packages announced in the Budget will deliver an extra $116.5 million per year in profit margin for providers – and clear the wait list by 2023 (without any growth in the 275,000-plus people estimates to be in a package at June 2023). StewartBrown also estimates that the $3.8 billion over two years allocated for introducing mandated minimum staff time for aged care residents by 2023 should be “adequate”. But the report finds the Government’s referral of an increase in aged care wages – combined with the Health Services Union case due to be heard by the Fair Work Commission in October this year – provides a real risk of an unfunded increase in wages.
“As wage costs represent up to 70% of the total costs of providing residential aged care services, any unfunded increase in wages would be a major impost on Providers and threaten the financial viability of many aged care homes.”
More aged care homes likely to close
The Government’s decision not to change the method of indexation for residential aged care subsidies also leaves it to the $10 Basic Daily Fee Supplement and the increase in the viability Supplement to improve funding to aged care homes.
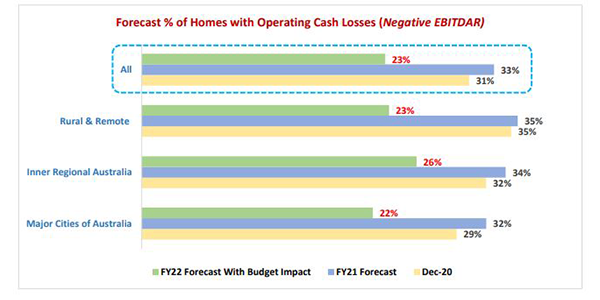
“Based on the December 2020 StewartBrown Survey, these two Budget measures are forecast to result in the average operating result for an aged care home to improve from a deficit of $9.95 per bed day (forecast FY21) to be a deficit of $0.38 per bed day for FY22. This would see the number of aged care homes with operating losses decline from 60% as forecast for FY21 to still be 45% of homes forecast for FY22.”
The report concludes that while the number of aged care homes operating at a cash loss will drop, 23% would still be in the red.
“This may lead to homes closing to ensure that the Provider remains financially viable overall. In this circumstance, it will be likely that the homes will not be transferred to another Provider and will permanently close potentially causing supply gaps.”
Tough times ahead then.




