Aged care demand rising fastest where workforce is thinnest

Australia’s aged care workforce is expected to fall short in many of the regions where demand for services will grow fastest, new modelling suggests, raising concerns about whether new services can actually be staffed.
Analysis from demographic data platform Informed Decisions warns that the biggest planning risk facing the sector is assuming national demand trends will play out evenly across local communities.
“The biggest oversight that we see is assuming that the average experience is what happens locally,” said its Chief Economist Rob Hall.

Planning based on national averages can lead to services being funded in areas where they cannot realistically operate because there are not enough workers to staff them.
Northern Beaches offers early warning
Sydney’s Northern Beaches illustrates the challenge.
Between 2026 and 2046, the area’s 65-plus population is forecast to grow by 38%, while the 80-plus cohort is expected to increase by 66%.
Demand for aged care and home care services will rise sharply.
Yet the workforce pipeline is already thin.
Around 25% of the local health care workforce is aged 55 or older, meaning a significant share is likely to retire over the same period that demand accelerates.
At the same time, 32% of health care workers commute into the region from other areas, reflecting housing affordability pressures that make it difficult for many staff to live locally.
Demand rising, workforce shrinking
The modelling highlights a fundamental challenge for the sector.
Across Australia, around 23% of the health care and social assistance workforce was aged 55 or older in 2021, and potentially nearing retirement age.
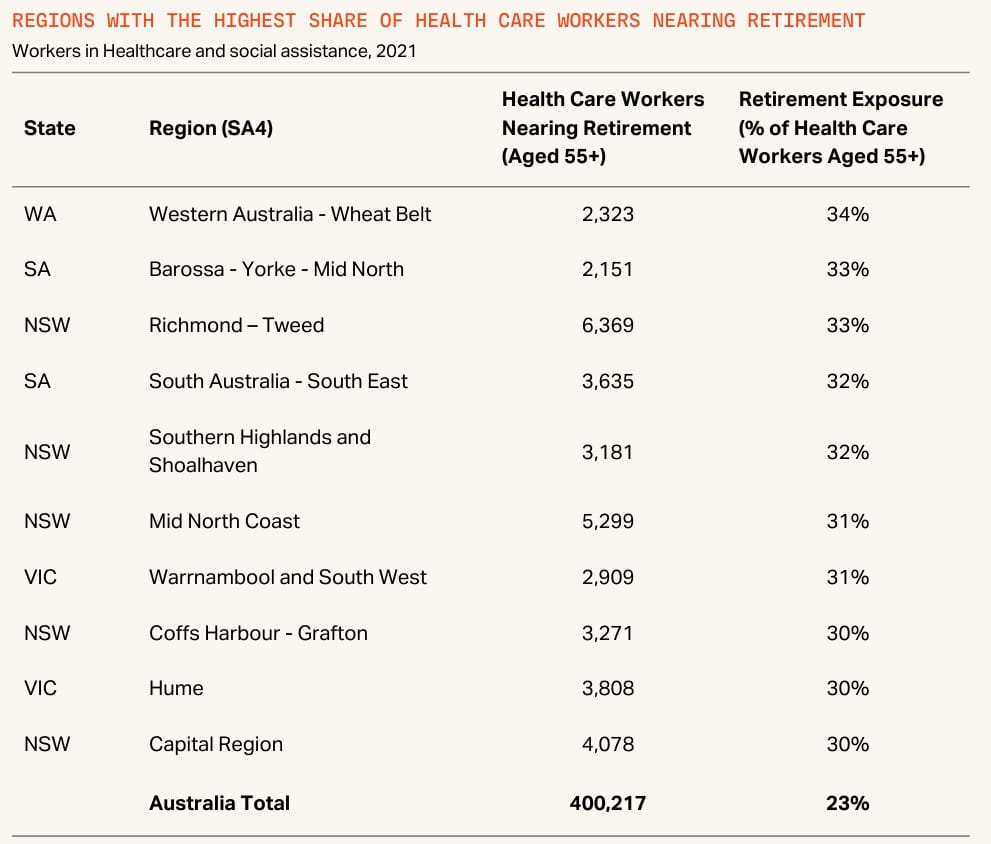
“If an organisation cannot secure enough staff, they simply can’t keep a facility running, regardless of how strong the demand may be in the area,” Rob said.
Aged care providers are also competing with hospitals, disability services and home care for the same labour pool.
Informed Decisions estimates the overlapping workforce across these sectors at around 460,000 people, meaning workers frequently move between systems depending on pay, rostering, workplace culture and travel time.
Workforce feasibility shaping investment
The report flags several types of regions where workforce shortages may constrain future service delivery:
- remote and inland communities with ageing populations and fewer younger workers
- coastal retirement hotspots experiencing rapid growth in older residents
- outer metropolitan growth corridors transitioning into older communities
- high-cost urban areas where housing affordability pushes workers away.
Housing affordability is already impacting workforce supply in several high-demand regions.
In some areas where aged care demand is rising fastest, median house prices are now 30 to 40 times the median annual income of a health care worker, limiting the ability of providers to recruit staff locally.
Rob said addressing the workforce challenge would require a combination of strategies rather than a single solution.
“It can’t be the one silver bullet,” he said.
“The response needs to include retention, new pathways into the care sector and productivity improvements.”





