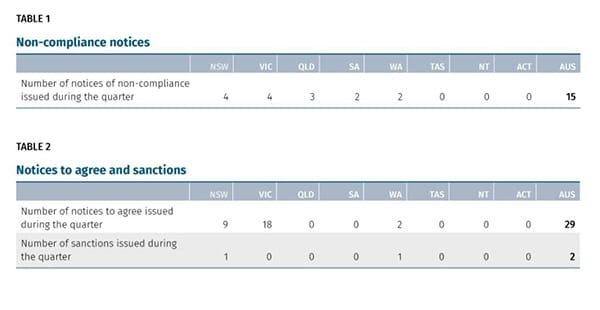
GPs put their own voluntary aged care standards out for second round of consultation – onus on providers to monitor prescription of psychotropic drugs
You can download the draft standards here
Last year, I reported in The Daily COMMISSION (September 6 2019, 14th edition) that the Royal Australasian College of General Practitioners (RACGP) was set to introduce their own standards for aged care homes to support the delivery of GP services – now the second review is here and there have been a few changes. You can download the draft standards here. Running to 73 pages, the draft outlines five key standards (under which there are a number of criteria) for aged care providers to follow:
- Resident care coordination – on providing access to and continuity of care for residents.
- Infrastructure, equipment, consultation spaces and treatment room – the equipment GPs require to provide services.
- Information management – the use of health record systems.
- Medication management – how medicines and treatments are managed; and
- Qualifications of the aged care home team (unsurprisingly the RACGP wants all staff to be accredited and certified in line with their profession).
There have been some key changes since the first draft was released last year. Understandably, providers had raised concerns about the availability of consultation spaces and treatments rooms – the new draft acknowledges this difficulty. The requirements for staff to be qualified have also not been increased to recommend staff-to-resident ratios – a key issue throughout the Royal Commission hearings and community forums – with feedback saying that the skills and qualifications are already captured in Aged Care Quality Standard 7: Human resources, according to Dr Louise Acland, Chair of the RACGP Expert Committee – Standards for General Practices (REC–SGP). “This was not the intended purpose of this Standard as it is out of scope to dictate the types of qualifications or mix of workforce an RACF should have,” she told NewsGP. Critically, the issue of psychotropic drugs in residential care – and the fact that GPs are responsible for prescribing them receives just two lines in the draft standards – and appears to shift the responsibility to aged care staff to ensure drugs are not misused. Under the heading ‘Pharmacotherapy review’ (the RACGP says the term “chemical restraints” does not adequately or appropriately reflect the potential role of short-term pharmacotherapy management of severe BPSD [behavioural and psychological symptoms of dementia), it states: “Medication safety is an important issue in RACFs. Overuse of antipsychotics and benzodiazepines in RACFs is of major concern, particularly when used as a form of chemical restraint.” “GP access to shared electronic health records and regular review of medicines is important to reducing the risks associated with these medicines. A three-monthly medical review of residents taking regular antipsychotics or benzodiazepines is required and ongoing use documented within a resident’s health record. Documentation of other nursing non-drug interventions must also be made.” In short, it is on providers to ensure that GPs have the information they need, conduct regular reviews of psychotropic medication and document any other measures taken. The Royal Commission has repeatably heard about the barriers facing GPs in delivering care in aged care homes including a lack of financial incentives, time, availability of nurses and record-keeping systems, but GPs who have appeared before the Commissioners are generally not questioned on their role in prescribing psychotropic drugs. Providers will have a chance to have their say however – consultation is still open here with the standards due to be piloted in aged care homes once COVID-19 restrictions are eased.