Grieving residents and families, traumatised staff and a lack of ‘command and control’: independent review of COVID-19 outbreaks at St Basil’s and Epping Gardens delivers lessons for providers
Now-Minister for Aged Care Services, Senator Richard Colbeck, had promised the Department of Health would release the long-awaited report into two of Victoria’s deadliest aged care COVID outbreaks before Christmas. Newly appointed Minister for...
Now-Minister for Aged Care Services, Senator Richard Colbeck, had promised the Department of Health would release the long-awaited report into two of Victoria’s deadliest aged care COVID outbreaks before Christmas. Newly appointed Minister for Health and Aged Care, Greg Hunt, delivered on this pledge – and the review contains several important takeaways for providers. 94 residents and 84 staff at St Basil’s Home for the Aged in Fawkner were infected with COVID at the height of Victoria’s second wave, with 45 residents passing away, while Heritage Care’s Epping Gardens had 103 residents and 86 staff infected, with 38 residents passing away. The 71-page report – commissioned by the Department at a cost of $211,778 and conducted by Professor Lyn Gilbert AO and Adjunct Professor Alan Lilly, both members of the Australian Health Protection Principal Committee’s (AHPPC) Aged Care Advisory Group (ACAG) – looked into the outbreaks and found both were complicated by a range of factors including difficulties in emergency planning and preparedness.
Residents, families and staff left traumatised
“These stark numbers [of infections and deaths] do not begin to convey the trauma and grief suffered by all residents … and the enormous impact on their families,” the Professors write. “They do not account for the distress of staff members, who knew and had cared for residents for long periods but were quarantined and obliged to leave them in the care of ‘strangers’”.
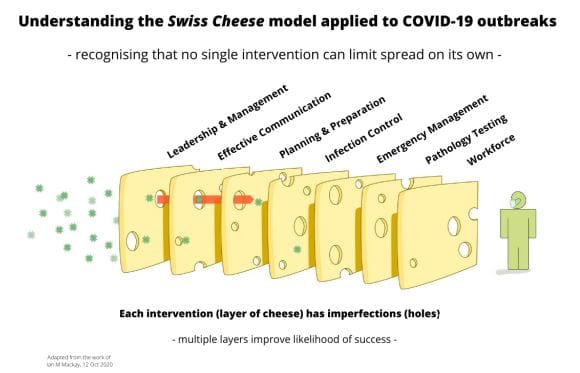
The authors use the analogy of several slices of Swiss cheese placed vertically and parallel to point out the gaps – or ‘imperfections in multiple slices’ as they call them – in the management of the outbreaks (pictured above).
Leadership and communication lacking
Leadership is highlighted throughout the report with the authors noting the facilities lacked a ‘command and control structure’ in their management. Communication and support from the Department and other agencies was also found to be lacking, along with communication with families and residents. Both facilities were also inadequately prepared in terms of outbreak management plans, infection prevention and control (IPC) and workforce.
No limits on hospital transfers
In particular, the report states that there should be no restriction on hospital transfers of residents on the basis of clinical need, while transfers in other circumstances should take place on an as-required basis. With many staff furloughed as positive cases of close contacts, the report says most of the workers hired to fill the gaps had little experience in aged care with many only speaking basic English.
“With little preparation or supervision, it is not surprising that many did not stay and those who did, were quite likely traumatised," they said.
Testing and contact tracing delayed
Delays in pathology testing, contact tracing and cohorting of residents and staff also had an impact. As the coroner is currently looking at some of the deaths at St. Basil’s – and both facilities are facing legal action over the outbreaks – the report acknowledges that the authors did not speak to all families, staff and management at the facilities. Both facilities also remain subject to a Notice to Agree (NTA) issued by the Aged Care Quality and Safety Commission (ACQSC) in July. The report concludes that there is an ongoing challenge to drive improvements across the aged care sector – but blame does not “drive improvement”.
“It is now imperative that the sector and those funding the sector, understand what more needs to be done to optimally mitigate such outcomes into the future. As one of the family participants said, ‘I hope these reviews do not gather dust like all the others into aged care’.”
Recent headlines suggest the media won’t forget at least – see the next story.





