Less money, lower staffing, more people in residential care: Royal Commission’s second research paper on international aged care systems shows where Australia is failing
Download the paper HERE
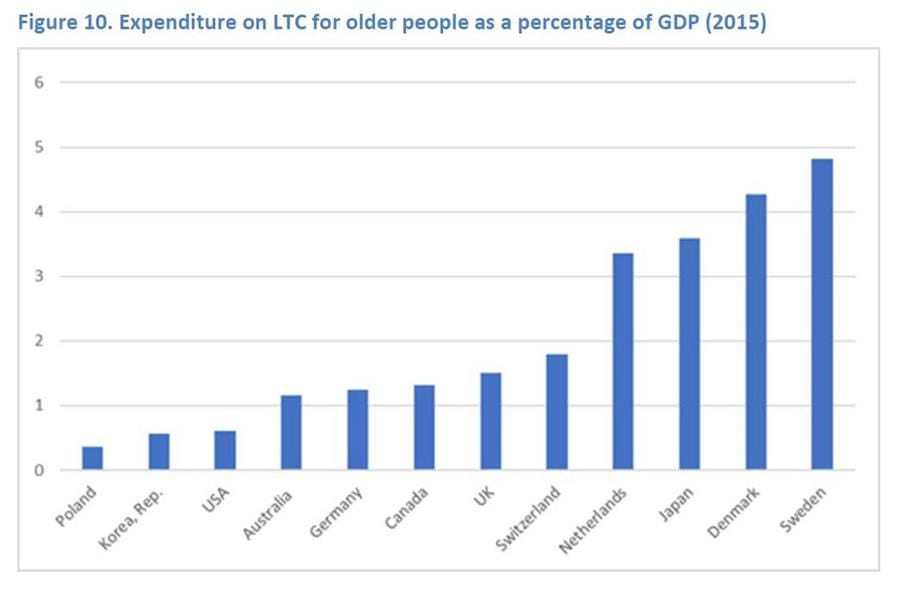
Australia spends just 1.2% of its Gross Domestic Product (based on OECD data) on aged care (pictured above) – far less than other comparative systems internationally, according to the Royal Commission’s second paper into how long-term care for older people is delivered in other countries. Unlike the Royal Commission’s first research paper ‘How Australian residential aged care staffing levels compare with international and national benchmarks’, there is no lightbulb moment in this paper – but there is a lot to learn. The 133-page literature review (with 16 pages of references) – titled ‘Review of International Systems for Long Term Care of Older People’ – was put together by the Rehabilitation, Aged and Extended Care Group, Flinders University and THEMA Consulting. The paper looks at aged care systems in 22 countries including Canada, Denmark, England, Germany, Japan, Korea, The Netherlands, Sweden and the United States as well as countries with limited systems like Vietnam, Indonesia, Central and South America and Sub-Saharan Africa. The report concludes Australia has plenty of room for improvement compared to other countries – and that Denmark and Sweden are likely to have the best systems. Why? Both spend more than 4% of their Gross Domestic Product (based on OECD data) on aged care. The countries with similar access to aged care as Australia i.e. where access is not means tested, consumers can choose their provider etc. spent an average of 2.5%. In contrast, Australia spends just 1.2%.
Denmark and Sweden also fund their systems through local government with federal grants and local taxes with a focus on delivering care in the home – again, a contrast to Australia which has one of the highest proportions of people aged over 80 in residential aged care – around 20% (pictured above). Unsurprisingly, staffing in Australia was also been found to be at the lower end of the scale internationally, both for total staffing and nursing in residential care.
“The number of nurses employed in home care settings in Australia may also be low in comparison to many other nations, including the USA. These data suggest further investigation of staffing levels in Australian LTC is warranted.”
The researchers also note Australia’s heavily regulated, single agency, inspection-based system is unlike many other countries which have multiple levels of responsibility and use mandatory reporting and publicly available data to ‘self-regulate’ providers.
“Sweden has a comparatively light regulatory approach but encourages professionalism and the use of clinical quality registers. These registers (e.g. dementia registers) link administrative data, allow benchmarking and facilitate transparency.”
However, none of the improvements that the researchers recommend be investigated for Australia are new ideas for the Royal Commission, namely:
- More support for home-based and informal carers including high-level Home Care Packages and better leave provisions.
- More involvement of local government in the regulation and monitoring of aged care services. “Higher levels of regulation may stifle innovation and there is little evidence that they improve care quality,” the paper says pointedly.
- Mandatory training and registration of aged care workers.
- Increased transparency in staffing levels.
- Mandatory reporting and public availability of quality of care indicators.
- Better integration with the health system to improve management of chronic conditions such as dementia.
- A stronger focus on rehabilitation and maintaining function.
- Incorporating the human rights principles in the Aged Care Standards.
The question you must ask is: why wasn’t this research done at the outset of the Royal Commission? Download the paper HERE.




