Third resident from St George Aged Care at Bexley, Sydney dies from COVID-19 as NSW Health cuts down on hospitalisations of vaccinated residents with the virus
Despite high vaccination rates among residents, the COVID-19 outbreaks in Sydney aged care homes are continuing to claim some lives. On Wednesday, it was revealed a third resident of the family-owned St George Aged Care at Bexley, 14km south of...
Despite high vaccination rates among residents, the COVID-19 outbreaks in Sydney aged care homes are continuing to claim some lives.
On Wednesday, it was revealed a third resident of the family-owned St George Aged Care at Bexley, 14km south of Sydney’s CBD, had died following a COVID outbreak.
The man, who was aged in his 90s, died at St George Hospital. Two other residents of St George Aged Care have died in the last week following an outbreak in August, which resulted from an infectious worker.
On Tuesday, it was made public that a resident, also aged in his 90s, of Advantaged Care’s Prestons Lodge in Prestons, 37km southwest of Sydney’s CBD, had died at Campbelltown Hospital after acquiring his infection at the facility. He had two vaccine doses and had significant underlying conditions, said NSW Chief Health officer Dr Kerry Chant The home recorded 12 new resident cases and two new staff cases in the last week, based on numbers released each week.
Aged care facilities in Sydney’s west and southwest have been told to provide on-site care for non-critical patients who have tested positive for COVID-19 due to a shortage of available beds in public hospitals, which increases the risk of the virus spreading.
In a statement on Friday, Uniting said seven residents of Uniting Edinglassie Penrith, 58km west of Sydney’s CBD, had been transferred to hospital with COVID-19. They were then advised by the public health unit and Nepean Blue Mountains Local Health District that no further clinically stable residents would be transferred.
“Aged care homes simply aren’t designed or funded to be able to provide hospital level containment and treatment of this virus, they need the support of the public health system,” said ACSA CEO Patricia Sparrow.
“We never want to see a repeat of the outbreaks we saw in Victoria last year. Hospitalisation and vaccinations are the only way to guarantee the best possible disease control and treatment. The Royal Commission backed this approach.”
NSW Health said residents with two vaccine doses who contract COVID-19 are only to be transferred to hospital if their condition “warrants admission”.
“Decisions on the most appropriate clinical care, including the location of that care, are made in consultation with clinical staff and residents and their families,” a NSW Health spokesman said.
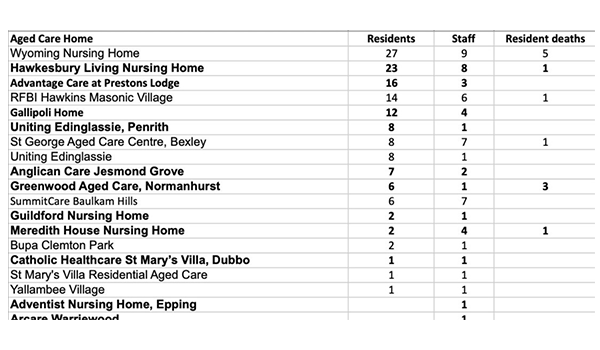
Latest figures made public show the incidence of COVID-19 in aged care homes is spreading in NSW with 18 more facilities recording active cases in the latest weekly reporting period.
However, numbers are still well below those seen in Victoria last year.
The total number of combined active cases in NSW facilities is 118 as of 8am last Friday including 72 in aged care residents and 46 in staff members.
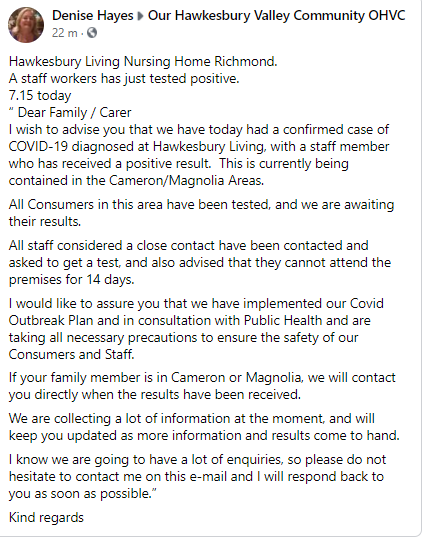
There is a larger outbreak at the Hawkesbury Living Nursing Home in Richmond, 63km northwest of Sydney’s CBD, which has 134 residents, with five more resident cases in the last week – bringing the total to 23.
Eight of Hawkesbury Living’s 184 staff have tested COVID-19 positive and are in isolation. At-risk residents have been transferred to Nepean Private, Nepean and Hawkesbury hospitals.
In Melbourne, an aged care worker who had two vaccine doses, has tested COVID-19 positive. Staff on the same shift are isolating but Victoria’s Chief Health Officer Professor Brett Sutton said on Wednesday that 95% of staff and residents were vaccinated.
In Queensland, restrictions on visitors to hospitals, aged care and disability facilities in the Logan area were also lifted on Wednesday.




