Aged care COVID admissions contributed to Australia’s largest outbreak among hospital staff, study finds
Over 260 Royal Melbourne Hospital staff were infected with coronavirus in July and August after a large number of COVID positive aged care residents were admitted in just a week, according to a new paper. The paper ‘A hospital‐wide response to...
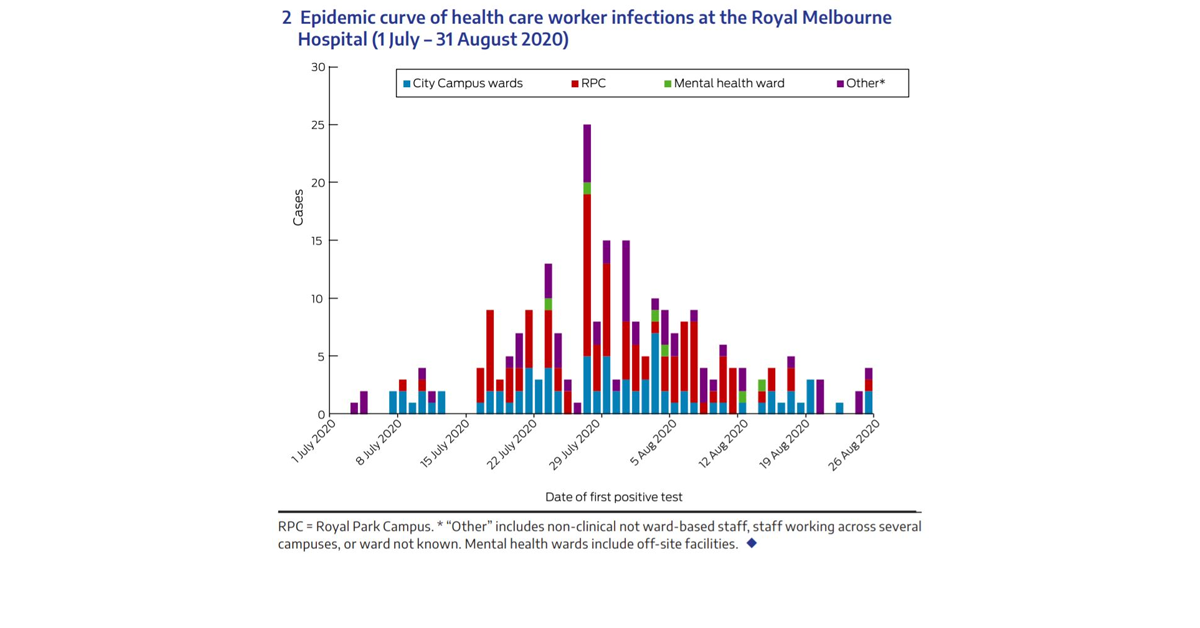
Over 260 Royal Melbourne Hospital staff were infected with coronavirus in July and August after a large number of COVID positive aged care residents were admitted in just a week, according to a new paper. The paper ‘A hospital‐wide response to multiple outbreaks of COVID‐19 in health care workers: lessons learned from the field’ – published in the Medical Journal of Australia yesterday – found the large, sudden influx of infected aged care residents to the 550-bed hospital – which has an additional 150 geriatric and rehabilitation beds at its Royal Park Campus – contributed to 262 cases among staff between 1 July and 31 August.
“The Royal Park Campus had the highest number of staff with COVID‐19, making up 40.8% (n = 107) of health care worker infections at the Royal Melbourne Hospital, despite this campus constituting about 10% of the total staff workforce at the hospital (acknowledging that some staff move between sites),” the study states. “Between 12 and 18 July, the campus received a large number of patients from external residential aged-care facilities… with COVID-19 outbreaks. These residents were positive at admission and managed with appropriate infection precautions (but) COVID-19 cases among staff rapidly escalated across all six wards after 16 July, peaking on 27 July. The peak number of patients with COVID‐19 at the Royal Park Campus was 60.”
Nurses and support staff most commonly infected
Of these 262 cases, two were admitted to intensive care, 15 (5.7%) needed inpatient care and 13 (4.9 per cent) received care through a ‘hospital in the home’ service. None of the staff died. Nurses were the worst affected, followed by support staff such as food and cleaning services and doctors, mostly trainees. No staff working in the hospital’s four attached aged care facilities were infected. The authors – led by RMH infectious diseases physician Kirsty Buising – pinpointed a lack of ventilation in the older buildings of the campus, its number of multi-bed spaces and high workloads of staff all, as factors contributing to the spread of the virus. The paper concludes that responses to COVID outbreaks in hospitals need to be multidimensional, with closure to new admissions, moving patients to separate rooms (where possible), managing the whole ward using increased precautions, deep cleaning, and voluntary testing of all patients and staff every three to four days all helping to curb the outbreak.