Home care hours have dropped 30 minutes in the last year, Grant Corderoy says – and it’s not only due to COVID
At LASA’s Ten Days of Congress this week, the StewartBrown Senior Partner revealed some shocking statistics on the state of home care – including that Level 4 package recipients are receiving just 50% of the care hours that they did 10 years...
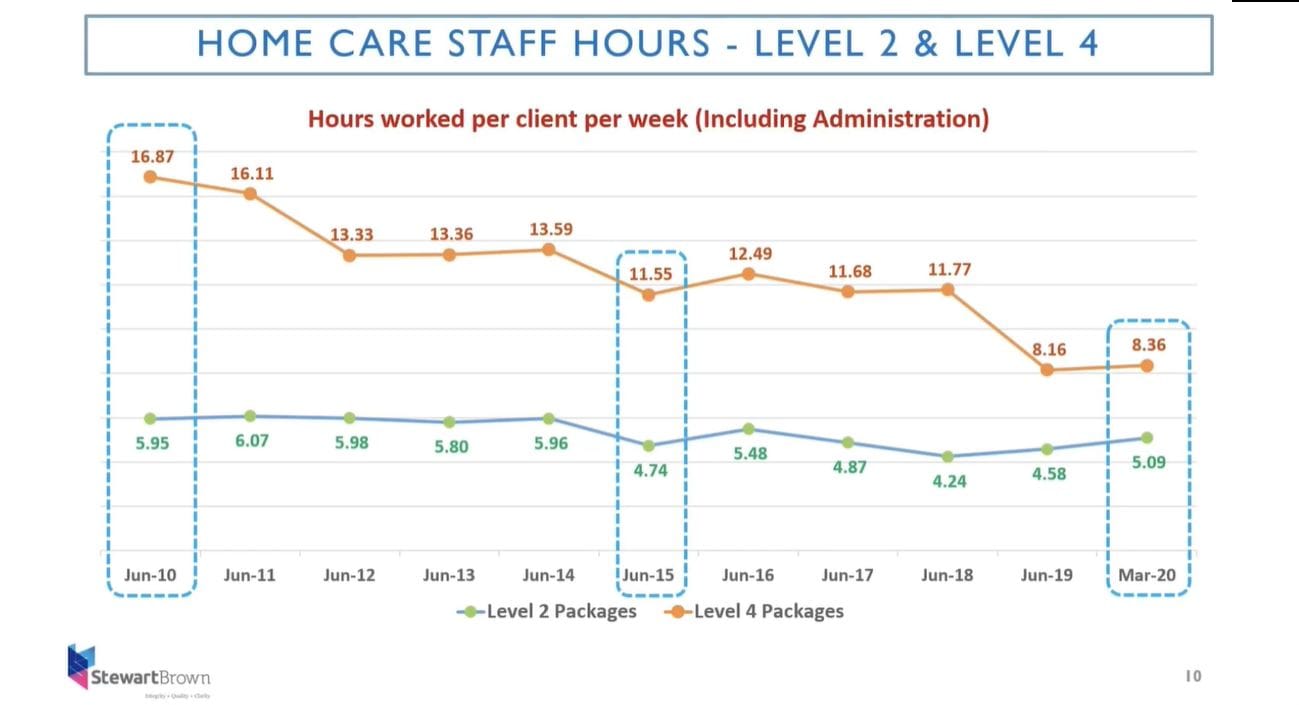
At LASA’s Ten Days of Congress this week, the StewartBrown Senior Partner revealed some shocking statistics on the state of home care – including that Level 4 package recipients are receiving just 50% of the care hours that they did 10 years ago. We asked Grant to explain StewartBrown’s numbers – and why they don’t lie. Take a look at their graph above which shows the actual number of hours for care delivery in total including administration. As we pointed out in Tuesday’s Daily RESOURCE, in June 2015, a Level 4 package provided an average of around 12 hours of care per week compared to under five for a Level 2 care recipient. Move forward to March this year and this gap has closed to three hours with a Level 4 now only providing 8.36 hours of care per week.
Direct care hours have dropped
Grant says based on their evidence, care hours for Level 1 and 2 packages – which offer services on par with the Government’s Commonwealth Home Support programme (CHSP) – have remained fairly consistent for the past decade. But at Level 4, the number of hours is declining – and this is bringing down the average number of care hours being delivered across the system. For the 12 months ending June 2020, direct service provision accounted for 4.12 hours of care a week according to StewartBrown’s data. Direct care by agency staff accounted for 0.23 hours, for a total of 4.35 hours spent on direct care.
Case management and admin hours stay the same
Case management and coordination made up 0.81 care hours, while administration services took up 0.48 care hours. In total, that’s an average of just 5.63 care hours delivered per week. Compare this to the 12 months ending June 2019 where direct care hours were an average of 4.59 hours a week, with agency staff making up 0.25 care hours, case management and coordination 0.80 and administration 0.47 for a total of 6.11 hours. As you can see from the figures, the use of agency staff and case management and administration costs have remained virtually the same – but direct care has seen a 0.49 drop or 30 minutes per week.
Consumers being over-assessed
As we reported in The Daily RESOURCE today, at least one home care provider has told us that their reduced hours are due to over-assessment; consumers spending their funding on goods rather than services; and the impact of COVID. Grant agrees that home care recipients are often being assessed on their future needs – not just their current ones – and this is the main contributor to the growing levels of unspent funds in the system – now at over $1.1 billion. However, he says the pandemic has not had a huge impact on care hours. For the nine months ending March 2020, direct service provision was 4.32 hours across all packages – this has since slipped to 4.12.
The drop in hours happening before COVID
But if you take COVID out of the equation, there was already a drop in care hours.
“If you compare the nine months ending March 2019 to the nine months ending March 2020, care hours went down 0.66,” Grant said. “The drop is not relational to COVID.”
The Senior Partner said he also would expect to see a drop in the level of unspent funds if consumers were directing their packages towards goods rather than services – which is not happening across the sector.
No margin for error
He adds that because of the size of their data set, the statistic margin for error is very low because they aggregate all of their data.
“We can tell if there is a major glitch,” he said. “There may be a difference between one provider and another but when you are looking at the statistics, this is an indication of what is happening in the sector.”
Potential funding for another 30,000 packages
So, if there has been a progressive drop in the number of care hours in home care, you have to ask the question: why is this happening? Grant points out he is not saying that providers are reducing their level of care – but he does say it is clear that care needs are not commensurate with funding levels. He argues that a more accurate assessment of care needs would help to redistribute funding to those in need of services – estimating that another 30,000 packages could potentially be funded. Given the Federal Government only found funding for 23,000 new packages in the recent Budget, should this be prioritized now before the Royal Commission delivers its findings?





