76% of aged care providers sanctioned from January to June 2020 were Not For Profits: Pride Living report
The aged care management specialist has released its report on non-compliance and sanction statistics from the first half of this year – and there are some surprises. The 10-page ‘Insights Report into Non-Compliant and Sanctioned Facilities’...
The aged care management specialist has released its report on non-compliance and sanction statistics from the first half of this year – and there are some surprises.
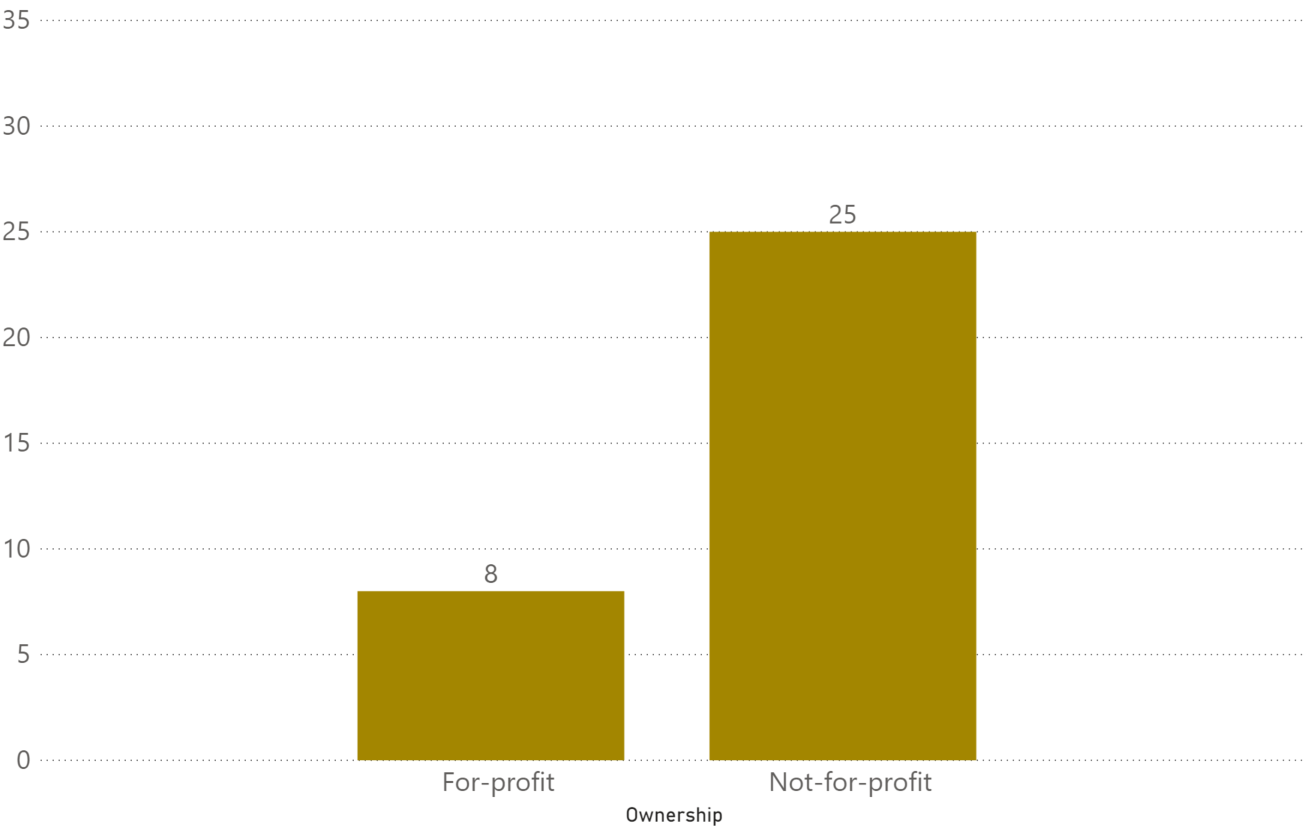
The 10-page ‘Insights Report into Non-Compliant and Sanctioned Facilities’ has found that of the 33 facilities issued with a non-compliance notice or, notice to agree or sanction, 25 (or 76%) were Not for Profits.
27 of the 33 were also located in major cities, and were more likely to be part of organisations with either 20-plus facilities followed closely by two to nine facilities.
Non-compliance higher despite fall in number of audits
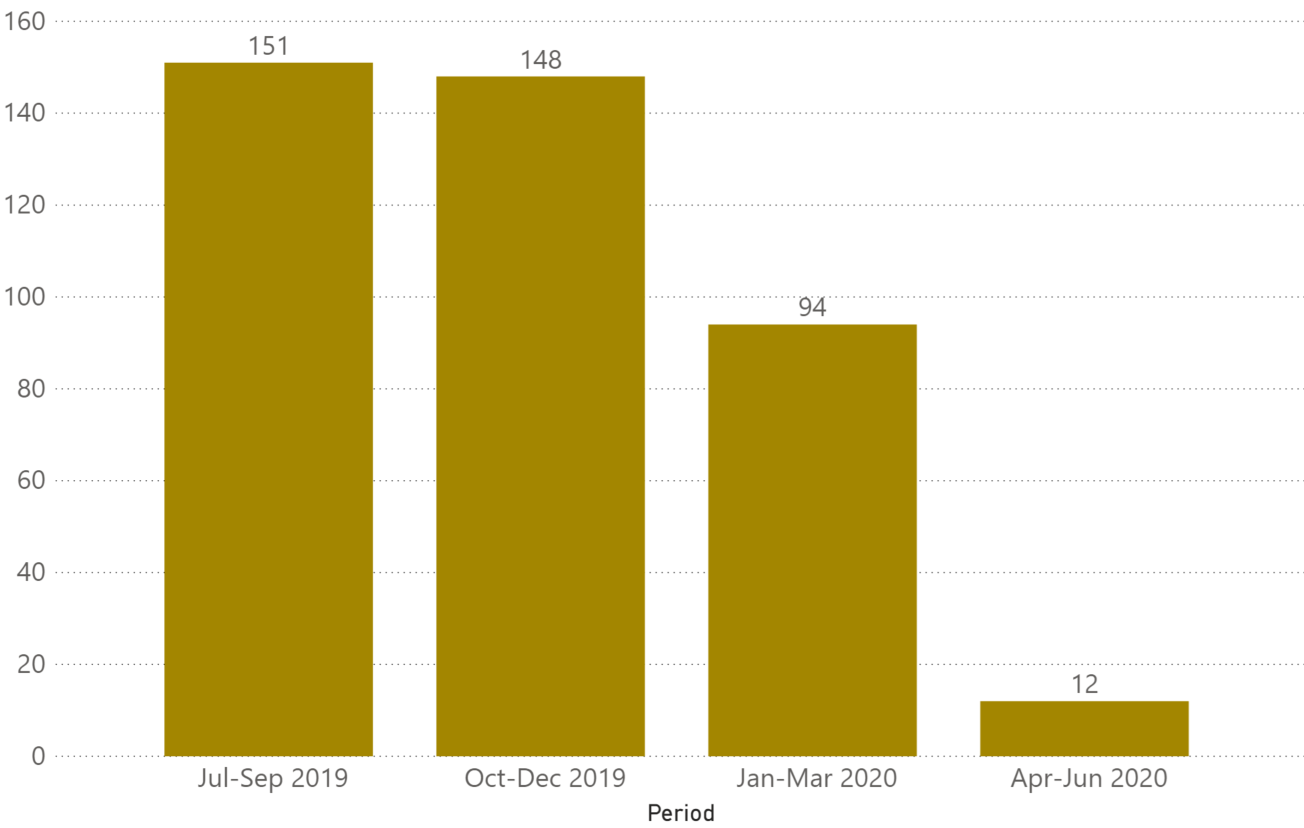
Rates of non-compliance are also higher despite of audits and contact assessments falling since the September 2019 quarter – well before COVID and the temporary halt in audits and assessments by the Aged Care Quality and Safety Commission (ACQSC).
Since July 2019, two in five (40%) of facilities that have been audited have been found to be non-compliant.
Assessment contacts between the September and March quarters also found one in six facilities (13-16%) were non-compliant, falling to 6% in the June quarter.
Clinical care still the main area of non-compliance
Safe and effective personal and clinical care continues to be the highest area of non-compliance, with 32 out of the 33 facilities found to have an unmet outcome in this standard.
The average number of unmet requirements had actually decreased since Pride’s previous non-compliance report.
However, a greater number of non-compliant facilities are failing standard 2, 7 and 8 – ongoing assessment and planning with consumers, human resources and organisational governance.
Non-compliances a result of leadership and governance
Pride concludes that COVID may be masking further deterioration in quality and compliance – and providers should focus on broadening their internal audit procedures as well as seeking second-party audits.
They also suggest the continued failings in Standard 8 indicate that the “governing bodies” have not been “effective” in implementing organisational and clinical governance systems.
In short, failures in leadership are responsible for falling standards of care.





